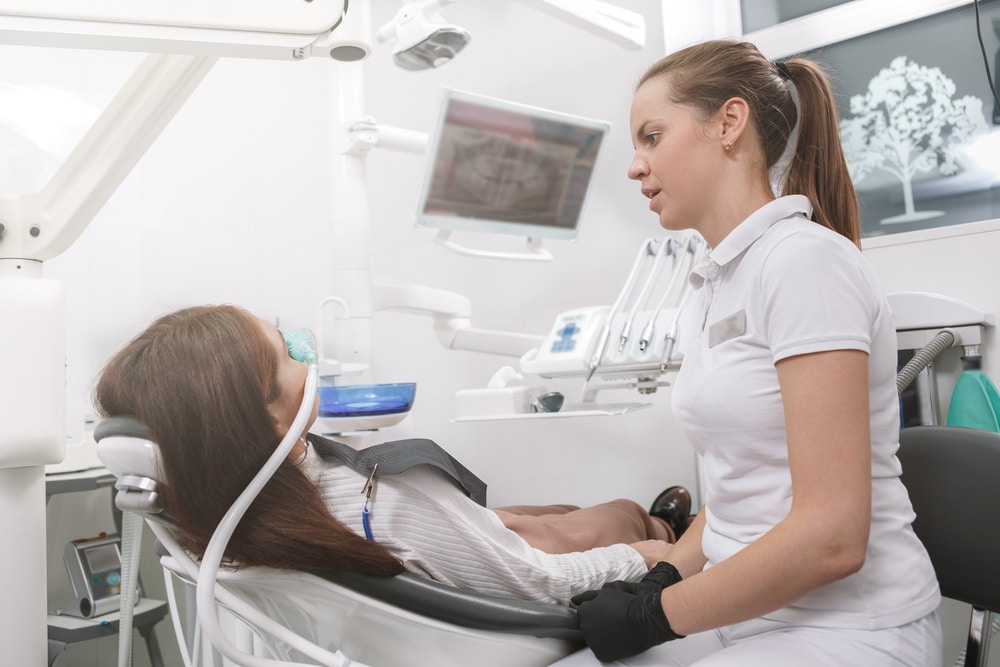
Are you feeling anxious about an upcoming dental procedure? Do you have a fear of needles or undergoing general anesthesia? If so, oral sedation may be an excellent option for you. However, preparing for oral sedation is essential to ensuring a safe and successful dental procedure.
In this article, we will provide you with tips and tricks to prepare for oral sedation, from patient assessment to postoperative care. By following these guidelines, you can reduce anxiety and achieve a relaxed state during the procedure. So, let’s dive into the world of oral sedation and discover how to prepare for a positive sedation experience.
Patient Assessment
Patient assessment is a critical aspect of preparing for oral sedation. It involves a comprehensive evaluation of the patient’s medical, dental, and psychological status to determine the suitability for sedation and identify potential risks.
Medical History Review
The first step in patient assessment is a review of the patient’s medical history. This includes any current medical conditions, past surgeries, allergies, and medications taken. The medical history review helps identify any contraindications to oral sedation, such as uncontrolled hypertension or a history of adverse reactions to sedatives.
It’s essential to obtain a complete medical history from the patient, including any medications they are taking, as some medications may interact with sedatives and cause adverse reactions. The medical history review should be documented in the patient’s chart and reviewed by the dentist or the dental team.
Allergy and Medication Screening
The next step is to screen the patient for allergies and medications. Allergies to medication or food can cause serious complications during sedation, and it’s crucial to identify them beforehand. Additionally, certain medications, such as beta-blockers and antipsychotics, may interfere with sedation and increase the risk of adverse reactions.
The screening process should include a comprehensive review of the patient’s medication list, including over-the-counter drugs, supplements, and herbal remedies. It’s also essential to identify any allergies the patient has and document them in the patient’s chart.
Physical Examination
A physical examination is essential to assess the patient’s general health status and identify any potential contraindications to oral sedation. The physical examination should include a review of vital signs such as blood pressure, pulse rate, and oxygen saturation levels.
The dentist or dental team should also examine the patient’s airway and assess their level of consciousness. Any findings should be documented in the patient’s chart, and any abnormalities should be addressed before administering sedation.
Psychological Evaluation
The final step in patient assessment is a psychological evaluation. Patients with anxiety, phobias, or other mental health conditions may require additional measures to manage their sedation. A psychological evaluation can help identify patients who require additional support during sedation and help the dental team develop a customized sedation plan.
The psychological evaluation may include an assessment of the patient’s mental health status, anxiety level, and previous experiences with sedation. Based on the findings, the dental team can determine the appropriate sedation level and develop a plan to manage any anxiety or phobias during the procedure.
Preoperative Instructions
Preoperative instructions are crucial for ensuring patient safety and a successful sedation experience. The dental team should provide detailed instructions to the patient before the procedure to prepare them for sedation and reduce the risk of complications.
Fasting Guidelines
Patients should fast before receiving sedation to reduce the risk of aspiration. The dental team should provide clear instructions to the patient on when to stop eating and drinking before the procedure. The fasting guidelines may vary based on the patient’s age, medical history, and the type of sedation used.
The following are general fasting guidelines:
- No food or drink for 6-8 hours before the procedure
- Clear liquids, such as water or apple juice, may be allowed up to 2 hours before the procedure
- Breast milk may be given up to 4 hours before the procedure
- Formula and solid foods should be avoided for at least 6 hours before the procedure
It’s essential to provide clear and detailed fasting guidelines to the patient and ensure they understand the instructions.
Medication Instructions
Patients may be taking medication for underlying medical conditions that may interact with sedatives. The dental team should review the patient’s medication list and provide instructions on any medication that needs to be discontinued or adjusted before the procedure.
Patients should also be instructed on any medication they need to take before the procedure, such as antibiotics or pain medication. The medication instructions should be provided in writing, and the patient should be instructed to bring their medication with them to the appointment.
Transportation Arrangements
Sedatives can impair a patient’s judgment and coordination, making it unsafe for them to drive or operate machinery. The dental team should instruct the patient to arrange for transportation to and from the appointment.
The patient should be advised not to drive or operate machinery for at least 24 hours after the procedure. They should also have a responsible adult accompany them to the appointment and stay with them for the remainder of the day.
Accompanying Person Requirement
Patients who receive oral sedation may require additional assistance and support during and after the procedure. The dental team should advise the patient to bring a responsible adult with them to the appointment.
The accompanying person should be informed of the sedation plan, postoperative instructions, and emergency procedures. They should be prepared to assist the patient during and after the procedure, including transportation and postoperative care.
Sedation Administration
Sedation administration is a critical step in the dental procedure that requires careful planning and preparation. The dental team must follow standard protocols and guidelines to ensure safe and effective sedation administration.
Dosage Determination
The dosage of sedative drugs used in the procedure depends on various factors, including the patient’s age, weight, medical history, and the type of sedation used. The dental team must carefully calculate the dosage of the sedative drug to avoid over-sedation or under-sedation.
It’s essential to follow the manufacturer’s guidelines for dosages and administer the drug slowly and incrementally, allowing time for the patient to respond to the sedative effect before administering more.
Monitoring Equipment Setup
Monitoring equipment is necessary to ensure patient safety during sedation. The dental team must prepare and set up monitoring equipment before the procedure, including:
- Pulse oximeter to monitor oxygen saturation
- Blood pressure monitor to monitor blood pressure
- EKG monitor to monitor heart rate and rhythm
- Capnography monitor to monitor carbon dioxide levels
The monitoring equipment should be checked and calibrated before use, and the dental team should be trained to use it correctly.
Sedation Onset Time Estimation
The onset time of sedation depends on the type of sedative drug used and the patient’s response to the drug. The dental team must estimate the sedation onset time to ensure the sedative effect has taken place before starting the procedure.
It’s essential to provide adequate time for the sedative drug to take effect and avoid administering more than necessary.
Emergency Kit Preparation
Despite careful planning and preparation, emergencies can still occur during sedation. The dental team must prepare and have an emergency kit readily available to manage any emergencies that may arise.
The emergency kit should include medications and equipment necessary to manage airway obstruction, respiratory depression, and cardiovascular collapse. The dental team should be trained in the use of the emergency kit and have a plan in place for managing emergencies.
Patient Monitoring
Patient monitoring is an essential component of dental sedation to ensure the patient’s safety and well-being during the procedure. The dental team must follow standard protocols and guidelines for patient monitoring to detect and manage any adverse events that may arise during sedation.
Vital Sign Assessment
Assessing vital signs is critical in monitoring the patient’s physiological response to sedation. The dental team must measure and record vital signs regularly, including:
- Blood pressure
- Heart rate and rhythm
- Respiratory rate
- Oxygen saturation
Any abnormal vital signs should be promptly addressed, and the dental team should be trained to manage emergencies.
Sedation Level Evaluation
Monitoring the patient’s sedation level is essential to avoiding over-sedation or under-sedation. The dental team must regularly evaluate the patient’s sedation level using a sedation scoring system.
The sedation scoring system should be used to determine the appropriate dosage of sedative drugs and monitor the patient’s response to the sedative effect.
Oxygen Saturation Monitoring
Oxygen saturation monitoring is critical to ensuring the patient’s adequate oxygenation during sedation. The dental team must use a pulse oximeter to continuously monitor oxygen saturation.
If the patient’s oxygen saturation drops below 90%, supplemental oxygen should be administered immediately.
Recovery Room Preparation
After the dental procedure, the patient should be closely monitored in a designated recovery area until they have fully recovered from sedation. The dental team must prepare the recovery room before the procedure, including:
- Providing a comfortable and quiet environment
- Ensuring adequate lighting and temperature control
- Having necessary equipment and supplies available, such as oxygen and suction
- Having trained personnel available to monitor the patient
The patient’s vital signs and sedation level should continue to be monitored until the patient is alert and oriented.
Postoperative Care
Postoperative care is essential to ensuring the patient’s complete recovery from dental sedation. The dental team must provide clear postoperative care instructions to the patient and their caregiver to avoid any complications.
Recovery Guidelines
After the dental procedure, the patient must be closely monitored in a designated recovery area until they have fully recovered from sedation. The dental team must follow the standard recovery guidelines, including:
- Monitoring the patient’s vital signs regularly
- Ensuring the patient is fully alert and oriented
- Providing a comfortable and quiet environment
- Administering oxygen and suction, if needed
The patient should be discharged only when they meet the standard discharge criteria.
Postoperative Instructions
The dental team must provide clear postoperative care instructions to the patient and their caregiver. These instructions may include:
- Eating and drinking guidelines
- Pain management instructions
- Oral hygiene instructions
- Activity restrictions
- Warning signs of complications and when to seek medical attention
The instructions must be provided in writing and explained thoroughly to the patient and their caregiver.
Follow-up Appointment Scheduling
The dental team must schedule a follow-up appointment with the patient to assess their recovery progress and ensure there are no complications. The follow-up appointment should be scheduled within a reasonable time frame, depending on the type and level of sedation used.
Patient and Family Education
Patient and family education are critical to ensuring a successful and safe sedation experience. The dental team must educate the patient and their caregiver on:
- The benefits and risks of sedation
- The procedure and sedation process
- The importance of following preoperative and postoperative care instructions
- The potential complications and warning signs
- The emergency contact information
By providing proper education and information, the dental team can ensure that the patient and their caregiver are well-informed and prepared for the sedation experience.
Conclusion
Preparing for oral sedation is crucial to ensuring a safe and successful dental procedure. By following the tips and tricks outlined in this article, patients and dental professionals alike can reduce anxiety and achieve a relaxed state during the procedure. From patient assessment to postoperative care, every step is critical to ensuring a positive sedation experience.
At Coquitlam Dental Group, we are committed to providing the highest quality dental care, including safe and effective oral sedation. If you are looking for a dental clinic that prioritizes your comfort and well-being, please visit us at Coquitlam Dental Group or give us a call at (604) 931-3133. We look forward to hearing from you!